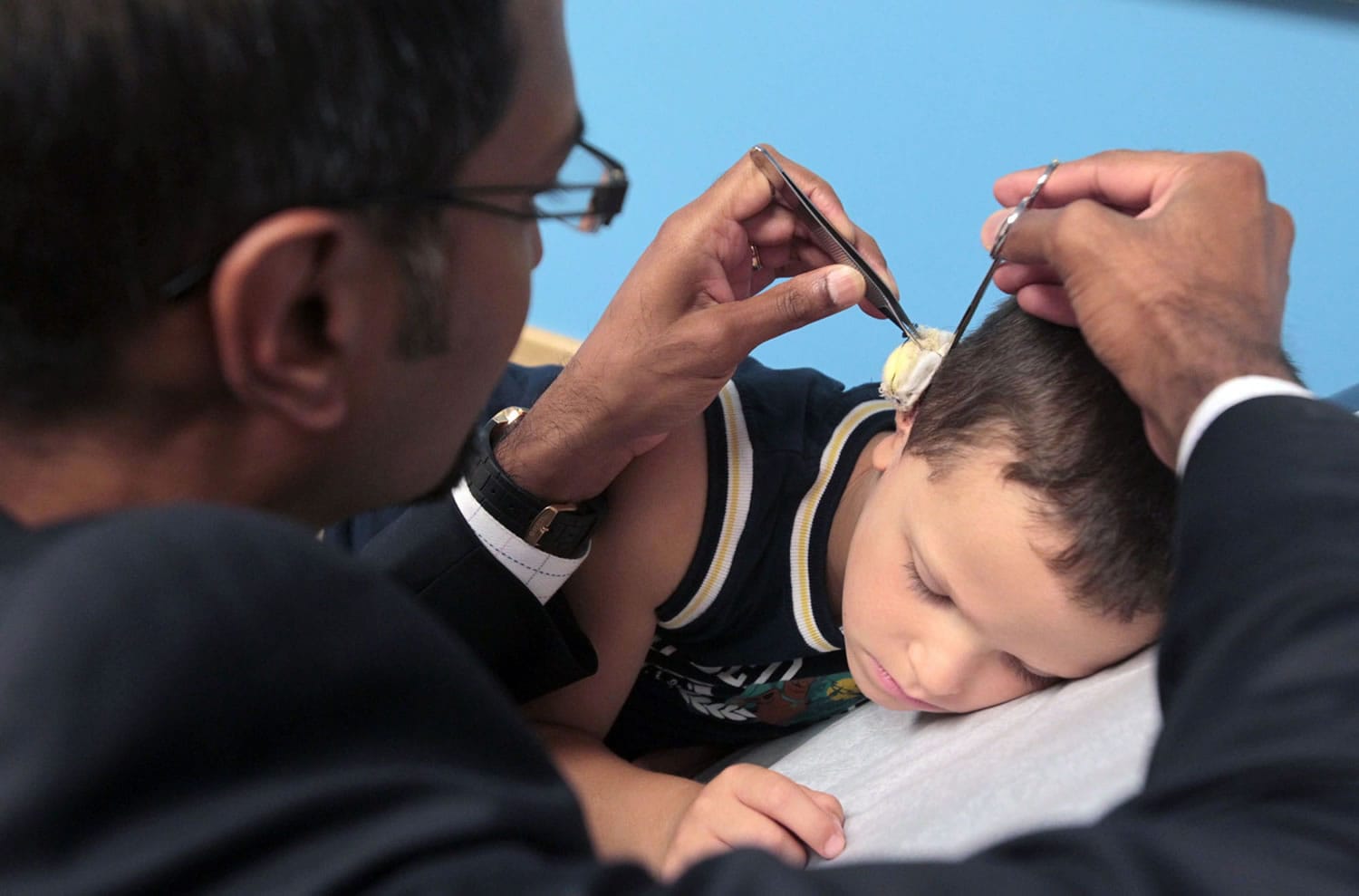
AKRON, Ohio — Kyle Figuray eyed the reflection of his ear with intense fascination.
For the previous three weeks, his right ear had been hidden from view by protective gauze after a second surgery this summer at Akron Children’s Hospital to correct a birth defect.
At a follow-up appointment, Dr. Ananth Murthy carefully removed the wrappings and held a mirror so the 5-year-old Wadsworth, Ohio, boy could see the results.
“It looks good,” Murthy said. “I’m very happy with it.”
For now, at least, children such as Kyle who are born with a birth defect that causes the outer ear and ear canal not to form correctly rely on a plastic surgeon to sculpt a new ear out of their rib cartilage.
But as Kyle continues to progress through the three required operations, research also is progressing at the University of Akron that could ultimately allow patients to grow their own perfectly shaped ear cartilage.
Initial results from attempts to grow ear cartilage with cells donated from Kyle’s underdeveloped ear tissue with his parents’ permission have been promising, said Dr. William Landis, the G. Stafford Whitby Chair of Polymer Science at the University of Akron.
Typically, the malformed ear cartilage is discarded as medical waste after it is removed during the first of three procedures to craft a new ear out of rib tissue.
Landis’ goal is to develop a technique in which the removed tissue — known as microtia cells — can be used to grow additional cartilage cells.
Those cartilage cells then could be seeded onto a biodegradable, biocompatible polymer scaffold that would provide the framework for a new ear.
“We wanted to verify that the microtia cells would develop in the same way and have similar properties as normal ear cartilage,” Landis said in an email. “What we have seen is we can grow the microtia cells and they look pretty good. And they appear to have properties resembling those of normal cells.”
Expanding research
Landis and members of his research team are continuing to study the growth of the microtia cells once they are seeded onto polymer scaffolds and implanted into special research mice. The researchers must determine whether the cartilage grown from microtia cells mirrors normal ear cartilage on a microscopic and biochemical level.
Landis also is exploring whether specific growth factors can be used to speed the cell growth.
The next steps will be repeating the experiments to make sure they go as expected more than once.
If these studies are successful, Landis then could approach the U.S. Food and Drug Administration about starting a clinical pathway toward patient use of the microtia-seeded scaffolds, possibly within five years or less.
The local research could be getting some support from an international biotech company. Landis and Murthy have been meeting with companies that are interested in potentially partnering with them on the project.
“We’re seeking support all the time,” Landis said.
In the meantime, Kyle has been relying on the artistic and medical skill of Murthy, a pediatric plastic surgeon at Akron Children’s, to create and perfect his new ear.
During the first procedure in January, Murthy and his team cut into Kyle’s chest and removed rib cartilage from near his sternum through a small incision. Murthy carved and sewed the rib cartilage into a shape that matched Kyle’s unaffected left ear.
Murthy then removed Kyle’s malformed ear cartilage, slipped the framework for the new ear under the skin and secured it with sutures.
Appearances
The results, though earlike, were two-dimensional. The ear was held by the skin flat to Kyle’s head without the typical separation from the scalp.
So during a second, hourlong procedure this summer, Murthy cut around the edge of Kyle’s new ear to free the ear cartilage from the boy’s head.
The surgeon used a thin, 2-inch by 2-inch skin graft taken from Kyle’s upper right hip to cover the now-exposed back of Kyle’s new ear. The skin on the side of his scalp was stretched behind the ear to create the natural fold.
“We created a little place where he can put his sunglasses on,” Murthy explained.
And, in fact, Kyle is required to wear glasses for several months, even though his vision is fine, so the groove between his ear and head doesn’t close.
Kyle will undergo a third, outpatient procedure later this year so that Murthy can add small details to the ear, such as an indentation where the ear canal normally starts.
The procedures aren’t improving Kyle’s hearing, only the appearance of his ear.
“I think he’s going to have a good result,” Murthy said.