For more information about ovarian cancer and the Ovarian Cancer Alliance of Oregon and Southwest Washington, visit the alliance website.
New research highlighting widespread flaws in ovarian cancer treatment is drawing attention across the country.
The research found only about a third of women diagnosed with ovarian cancer receive treatment meeting best practices standards. But one local specialist says Clark County providers, and patients, are faring better.
Symptoms of ovarian cancer include:
• Bloating
• Pelvic or abdominal pain
• Difficulty eating or feeling full quickly
• Urinary symptoms (urgency or frequency)
See your physician if these symptoms are unusual for you and occur almost daily for more than a few weeks.
Source: Ovarian Cancer National Alliance
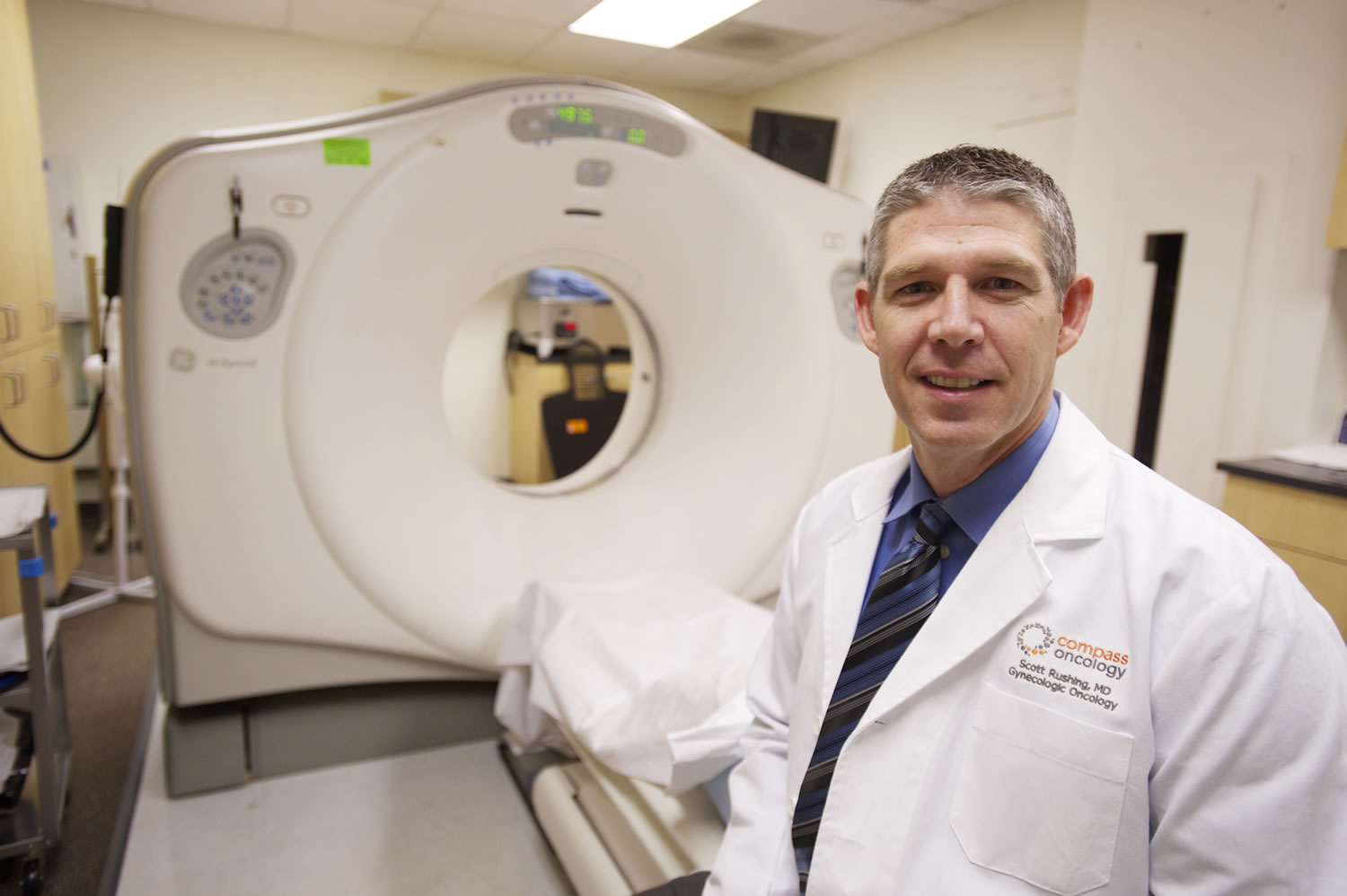
“In Clark County, we’re doing pretty good,” said Dr. Scott Rushing, a gynecologic oncologist at Compass Oncology. Rushing is one of only two gynecologic oncologists, who specialize in treatment of cancer in the female reproductive system, in Clark County.
The research points to two areas where cancer care is falling short: surgery and chemotherapy.
First, too few women are having their surgical procedures performed by gynecologic oncologists. Instead, women are having their regular gynecologist or the obstetrician who delivered their children perform the procedure. Those physicians may not have the experience or expertise of specialists, Rushing said.
Ovarian cancer surgery is aggressive, he said. Surgeons remove not only the large tumors on the ovaries but all visible traces of the disease, a surgical procedure called debulking. That may mean removing a segment of the colon, the spleen or part of the small intestine in order to reduce the amount of cancer remaining.
“Survival depends on how much tumor is left,” Rushing said.
The other problem, according to the research, is many women don’t receive the most effective type of chemotherapy.
Intraperitoneal, or IP, therapy, which injects the drugs directly into the abdomen, is the most effective chemotherapy regimen for ovarian cancer. The treatment is more toxic than standard intravenous chemotherapy, and not all patients can tolerate it. Those who can, however, typically add months to their lives, Rushing said.
A 2006 study found ovarian cancer patients who had IP therapy survived an average of 67 months, as opposed to about 50 months with standard chemotherapy.
“There’s a survival advantage,” Rushing said, adding that most of his longtime survivors received IP therapy.
For the most part, Rushing said, Clark County women who are diagnosed with ovarian cancer are being referred to the appropriate specialists and, when they’re a candidate, are given the option of IP therapy.
In Clark County, there’s a good line of communication between physicians and specialists. It’s not unusual for local obstetrician/gynecologists to call Rushing to consult with him about a patient. And, for the most part, patients are sent to Rushing before the cancer has even been confirmed.
Physicians don’t have any way to screen women for ovarian cancer. That means the cancer typically goes undiagnosed until it’s entered later stages, when the tumors have grown big enough to cause discomfort and pain, Rushing said.
About 80 percent of ovarian cancer cases are advanced stage. At that point, the cure rate is only about 15 percent, Rushing said. But aggressive surgery and chemotherapy can extend life, he said.
Symptoms of ovarian cancer include:
• Bloating
• Pelvic or abdominal pain
• Difficulty eating or feeling full quickly
• Urinary symptoms (urgency or frequency)
See your physician if these symptoms are unusual for you and occur almost daily for more than a few weeks.
Source: Ovarian Cancer National Alliance
Vancouver resident Diane Rader O’Connor, an 11-year ovarian cancer survivor, underwent aggressive treatment when she was diagnosed in January 2002 at age 57.
When O’Connor’s gynecologist discovered the grapefruit-sized growth on her left ovary during an annual exam, she immediately referred O’Connor to a gynecologic oncologist in Portland.
O’Connor underwent surgery two days later. She also completed six sessions of intravenous chemotherapy (IP therapy wasn’t widely used in 2002). She’s been cancer-free since.
After learning about ovarian cancer survival rates and realizing how little people knew about the cancer, O’Connor decided to take action. About six years ago, O’Connor and her friend, Diane Elizondo, co-founded the Ovarian Cancer Alliance of Oregon and Southwest Washington, a partner member of the Ovarian Cancer National Alliance. The alliance educates women and medical students about ovarian cancer and gynecologic oncologists; provides networking and support for cancer survivors; and advocates for policies and funding for ovarian cancer research.