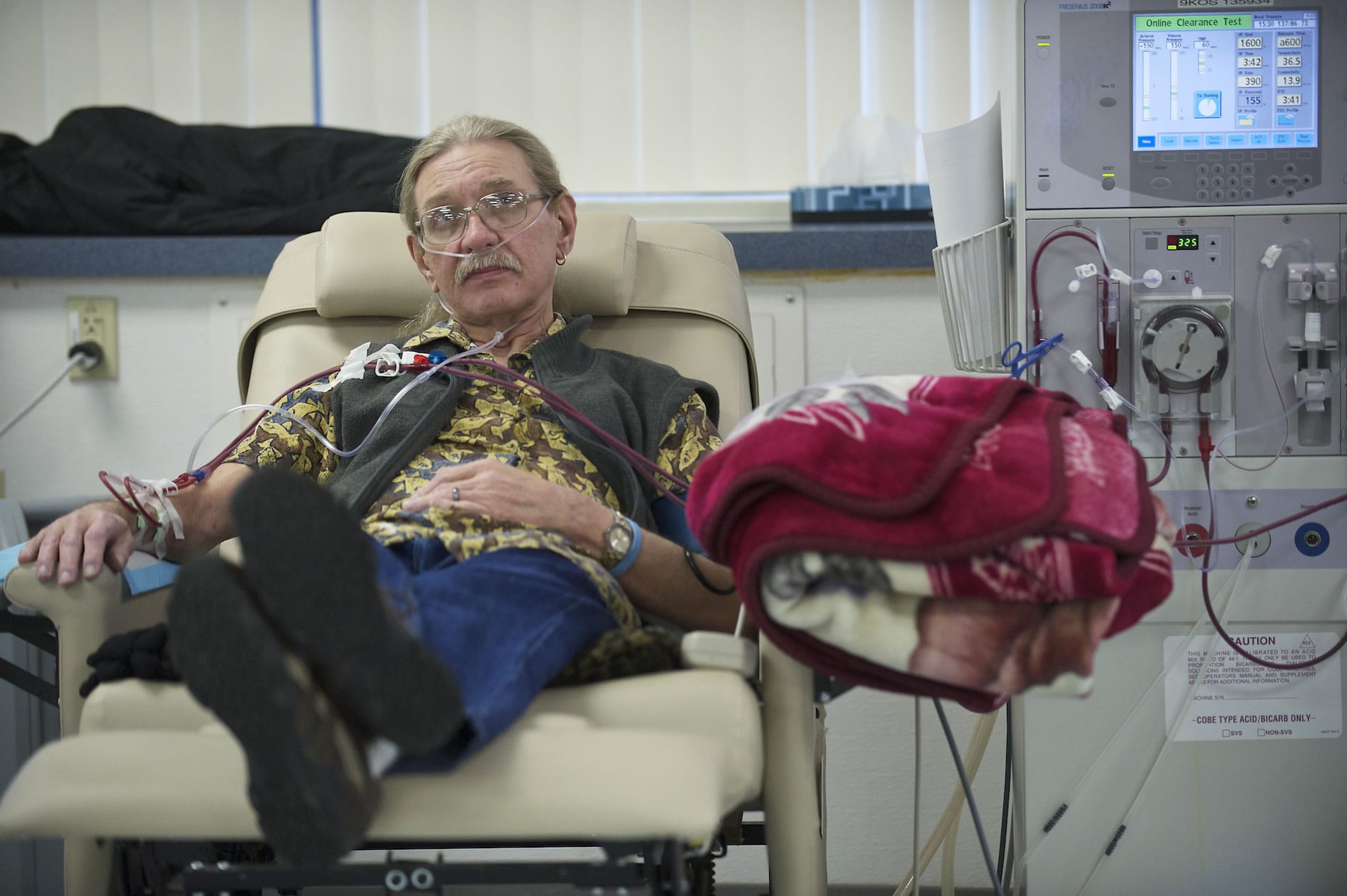
For nine months, Larry Sperry was a creature of the night. But not by choice.
At the time when most people would turn in for the night, Sperry was heading to the dialysis center. As most people slept soundly in their beds, Sperry sat in his chair, arm tethered to the dialysis machine, and watched infomercials.
“There’s not a lot of great TV from 11 (p.m.) to 3 (a.m.),” Sperry said.
But he didn’t have a choice. The Vancouver man has end-stage renal disease. His life depends on those several-hour dialysis treatments three days a week.
As demand for dialysis treatment increases in Clark County, dialysis centers already operating at capacity are adding additional shifts during the middle of the night to keep up with the need.
Like Sperry, Adrian Miller of Vancouver was assigned to a nocturnal shift. Miller, who is in renal failure, received treatment from 10:30 p.m. to 2:30 a.m. for eleven months. Two weeks ago, he was finally switched to a day shift.
“I was absolutely shocked,” Miller said. “When they gave me the times, I thought they were mistaken. I thought it was a typo.”
The middle-of-the-night shifts may, eventually, be a thing of the past.
Clark County’s two dialysis providers, DaVita and Fresenius Medical Care, are tied up in the state regulatory process that will ultimately grant one company permission to build another treatment center.
DaVita currently operates one local dialysis center near Westfield Vancouver mall. Fresenius operates two Clark County centers — one in Salmon Creek, the other in Cascade Park.
In order to build new centers, dialysis providers must apply for a certificate of need from the Washington State Department of Health. The certificate of need program requires certain health care providers — including hospitals, nursing homes, kidney dialysis centers and hospice care centers — to get state approval before building facilities or offering new services.
In January 2011, both dialysis companies submitted proposals to build a new facility in Battle Ground. The state reviewed the applications and on Oct. 31, 2011, granted DaVita the certificate of need, said Janis Sigman, certificate of need program manager.
Fresenius appealed the state’s decision. After reviewing the appeal and discovering additional information not included in the original application, the state reversed its decision and awarded the certificate of need to Fresenius, Sigman said.
DaVita appealed the state’s new decision and a hearing with an adjudicative clerk has been scheduled for mid-March, Sigman said.
In January, Sen. Don Benton, R-Vancouver, introduced a bill that would eliminate the certificate of need review for all health care facilities except hospitals. The Senate Committee on Health Care held a public hearing on the bill — Senate Bill 5017 — on Jan. 29.
Even if the bill does pass during this legislative session, it wouldn’t go into effect until 90 days after the session ends in late April.
Number of patients on rise
In the meantime, the number of Clark County dialysis patients is continuing to increase.
In March 2011, 325 people received treatment in Clark County’s three dialysis centers. By March 2012, that number had climbed to 353, according to data compiled by the nonprofit Northwest Renal Network.
Dialysis patient numbers have been steadily increasing steadily in the Northwest and across the U.S. for years, said Chad Lennox, executive director of the Northwest Renal Network.
Many centers across the U.S. are offering nocturnal shifts as an option for patients who may prefer the late-night treatments, Lennox said.
In Clark County, the shift is out of necessity, not choice.
The local dialysis centers were operating at 80 percent or higher capacity when they applied for the certificate of need. Now, two years later, they’re all at, or above, capacity, according to the centers.
To meet demand, Fresenius added a fourth shift that offers overnight dialysis six days a week. DaVita also added late-night treatment to accommodate more patients.
While the shift helps meet need, patients say it also puts additional strain on them and their families.
For Sperry, the dialysis schedule interrupted his other daily schedules — eating, sleeping and medication.
Unlike many other patients, Sperry couldn’t fall sleep during dialysis. That meant he didn’t go to bed until after 3 a.m. and didn’t wake up until noon or later. As a result, he was eating meals at unusual times and didn’t always take his medication at the appropriate time because some need to be taken with meals.
“I couldn’t have taken it much longer on the night shift,” the 63-year-old said. “It was really screwing up my life.”
And since Sperry couldn’t drive himself to and from treatment, he relied on his wife for transportation.
“It was ruining not only my life, but my wife’s life as well,” he said.
The treatment schedule made Miller, 41, once again dependent on his parents.
“The biggest obstacle is once you go on dialysis, especially at that time, you can’t work,” he said. “I went from a mortgage broker making good money to nothing. I’m 41 years old, and I had to move back home.”
Both Miller and Sperry said they are relieved to now receive treatment during daytime hours.