What: Creekside Dental is hosting an event to help the Campbells cover medical and other related expenses.
When: 5 to 8 p.m. Feb. 6.
Where: East Fork Cellars at the Slocum House, 605 Esther St., Vancouver.
Details: Free wine tastings and appetizers. Wine by the glass or bottle for purchase.
Other efforts: http://bit.ly/L7It5B
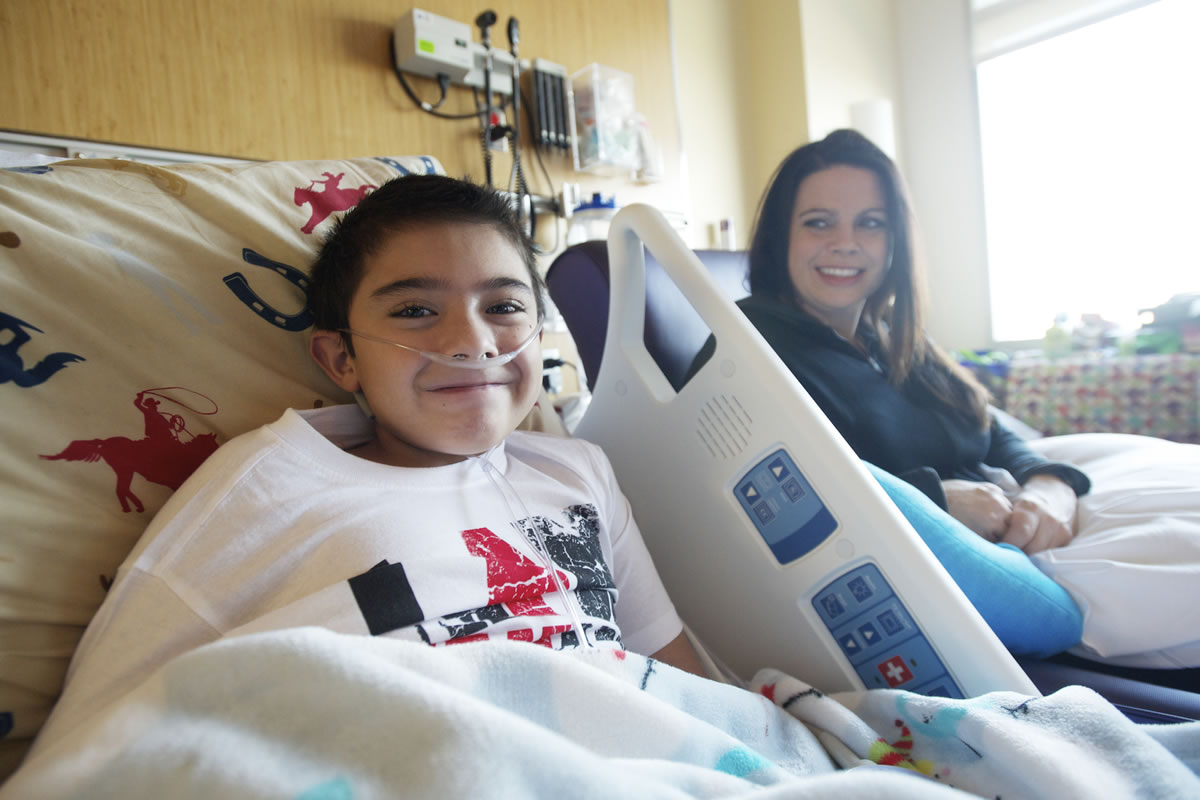
PORTLAND — Alex Campbell’s room is quiet. The natural light from the Portland sky illuminates the room. Handmade get-well cards sit on a shelf across from his bed. Those, he points out, were made by his friends at Salmon Creek Elementary School, where Alex is in fourth grade.
Alex, 9, leans back in his bed, his head cushioned by a pillow covered with images of cowboys and horses. A fleece snowman blanket is draped over his legs. His mother, Mandy Campbell, sits in a chair by his side, where she plans to stay until her youngest child is better.
What: Creekside Dental is hosting an event to help the Campbells cover medical and other related expenses.
When: 5 to 8 p.m. Feb. 6.
Where: East Fork Cellars at the Slocum House, 605 Esther St., Vancouver.
Details: Free wine tastings and appetizers. Wine by the glass or bottle for purchase.
Other efforts: http://bit.ly/L7It5B
Just a few months ago, Alex was his normal, energetic self.
“Alex is so active and athletic, and loves sports,” Mandy said. “He’s just always going.”
“How quickly it happened,” she added as her voice trails off.
These days, Alex spends most of his time in his hospital bed. A thin, clear tube runs beneath Alex’s nose, supplying additional oxygen.
“I kinda get all dizzy if I get up to the bathroom,” Alex said.
“I hate having oxygen,” he added, with a sideways smile that doesn’t quite mask the sadness in his voice.
Before he got sick, Alex liked to play football with his older brother. He loved playing soccer. But because those activities aren’t possible, Alex finds other ways to pass his time.
Sometimes, he plays with Legos on a lunch tray. Other times, he uses his tablet computer to shop on the Internet. He responds to text messages from friends. He watches TV.
On Saturday, he sat in his bed and watched the Seattle Seahawks defeat the New Orleans Saints. His eyes grow big when he talks about his favorite team.
“Marshawn Lynch,” he said, a big smile spreading across his face.
He just hopes the team plays well against a “pretty competitive” San Francisco 49ers team this weekend. Alex plans to watch the Seahawks game from his hospital bed again. But rather than a Portland hospital bed, he’ll be in a Houston hospital bed.
On Wednesday morning, Alex and Mandy boarded a medical transport plane and headed to Texas Children’s Hospital. There, Alex hopes to be the recipient of a double lung transplant. It’s unclear how long it will take to get a transplant. Sooner rather than later, they hope.
“We don’t have time to wait,” Mandy said.
The only option
Alex has always had allergies. His constantly stuffy nose sometimes left Alex short of breath when he was active. After taking a short break, Alex would usually catch his breath.
But in early November, Mandy noticed Alex was getting short of breath more frequently. Maybe, she thought, he has mild asthma.
So Mandy took Alex to his pediatrician’s office. There, they discovered the amount of oxygen in his blood was low. So low, the medical staff used several different machines to test Alex, believing their machines weren’t operating correctly. If the machines were correct, the boy wouldn’t be standing there before them, they told Mandy.
Mandy later took Alex to the emergency department at Legacy Salmon Creek Medical Center. They immediately transferred Alex to Randall Children’s Hospital at Legacy Emanuel in Portland.
There, Mandy learned Alex is facing a condition more severe than asthma.
Alex’s pediatric pulmonologist, Dr. William Nichols, said Alex has a condition called diffuse pulmonary arteriovenous malformation. Typically, unoxygenated blood goes through the lungs to get oxygenated. In Alex’s case, his blood bypasses through passages called shunts and doesn’t get oxygenated, Nichols said. As the shunts get bigger, Alex’s condition worsens because less and less blood is getting the necessary oxygen, he said.
The condition is an abnormality caused by a genetic disorder of the blood vessels, called hereditary hemorrhagic telangiectasia or HHT.
“HHT is fairly rare,” Nichols said. “This manifestation is even more uncommon.”
After four or five days in the Portland hospital, Alex was allowed to go home. He toted an oxygen tank around wherever he went, including school.
Alex continued to struggle, even with the oxygen. During a follow-up appointment on Christmas Eve, Nichols told Mandy that Alex needs a double lung transplant.
“A transplant is our only option,” she said.
On his next appointment, on Jan. 7, Alex’s blood oxygen saturation levels were so low, doctors admitted him to the hospital again and immediately began work to get Alex transferred to Texas Children’s Hospital for a transplant.
The Houston hospital has a lung transplant program that’s among the largest in the world and is one of only two centers performing more than 10 pediatric lung transplants each year, according to the hospital’s website.
At the Houston hospital, Alex will be evaluated and placed on a waiting list based on the severity of his condition.
“To me, he seems like he should be pretty high on the list,” Nichols said. “But it’s hard to predict.”
According to the hospital website, the lung transplant program has a median wait time of less than four months.
While Alex’s condition appeared to come on quickly, Nichols suspects it’s been progressing over the last several months or years. In just the last couple months, since Alex became a patient, Nichols has seen his condition worsen.
“He’s pretty low in his oxygen at all times, despite giving him extra oxygen,” Nichols said.
Normally, a person’s oxygen saturation level is between 98 and 100 percent, Nichols said. Alex’s oxygen saturation is in the mid-80s — and that’s with the supplemental oxygen. Without it, Alex is in the 60s or 70s, Nichols said.
Without a transplant, the condition will likely continue to progress and Alex’s oxygen saturation levels will continue to drop, Nichols said. How quickly that could happen is unclear, he said.
The transplant is a significant procedure with serious risks, but it appears to be Alex’s only option, Nichols said.
And it’s the only way Alex can return to his energetic, athletic self.
“I like to play football with my brother,” Alex said. “But I can barely even do it because I get winded.”