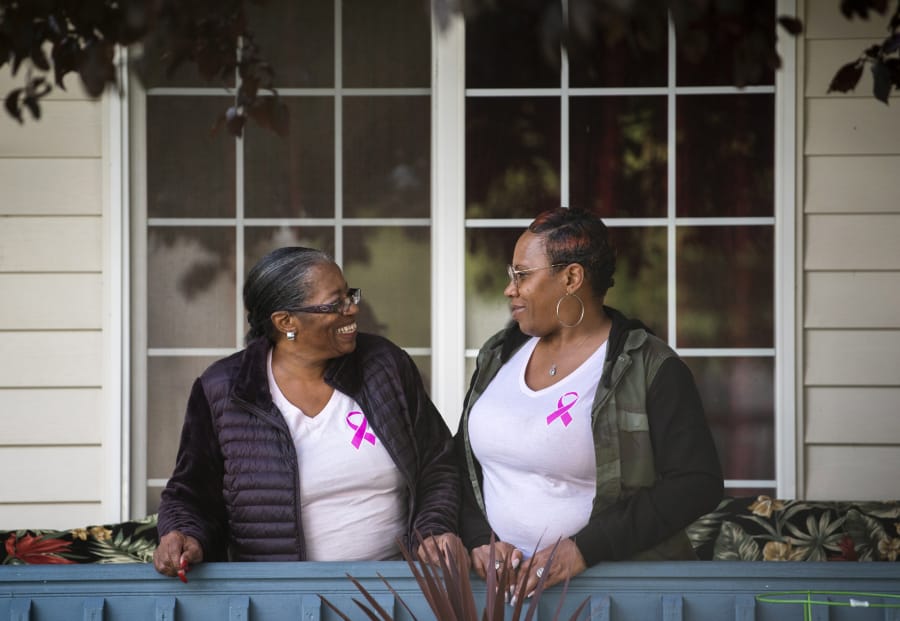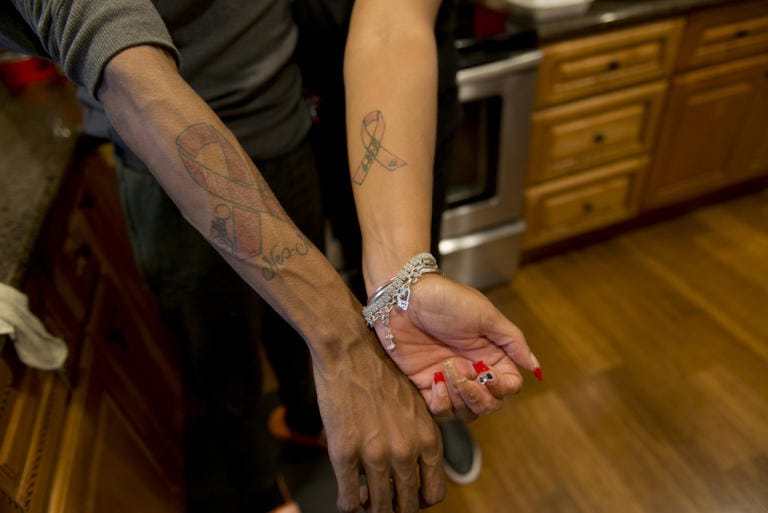Children play downstairs. Football is on TV. Laughter fills the home. Spaghetti, ribs and fried chicken are almost ready for consumption.
About 30 family members of Della Frazier, 71, and her daughter, Zsaneen Kennedy, 51, are gathered throughout Kennedy’s Vancouver home. Reminders of what has passed are sprinkled around the home.
A “keep calm and fight on” banner draping a doorway. A big pink breast cancer ribbon on Kennedy’s shirt. A breast cancer bumper sticker on a car outside. Signed pink boxing gloves given to Kennedy for a “cancerversary” party rest in the living room.
Before the family starts its Sunday feast in late September, loved ones circle together, hold hands and pray. Sherani Hill, one of Kennedy’s sisters, says the prayer.
“We thank you to see a day that was never promised,” Hill said.
Kennedy and Frazier are breast cancer survivors. Kennedy was diagnosed in February 2018. Her mother’s diagnosis followed in June. Kennedy’s last radiation treatment was the same day her mother had a lumpectomy — June 28, 2018, a date tattooed on Kennedy’s forearm.
Both women have finished treatment — Frazier still takes a pill. Yet the family still feels the mark of breast cancer. Once or twice a month, they host a Sunday dinner, where everyone can get together like they did in late September. It was at a similar family gathering when Kennedy told her family she had been diagnosed with breast cancer.
The environment that day was teary. People were in shock, trying to process the information, Kennedy said. Breast cancer runs in the Frazier and Kennedy families. Kennedy’s mother-in-law, Rosa Kennedy, contracted breast cancer in 2002. Rosa Kennedy has had an aunt and cousins die from it.
That prevalence is no surprise when considering statistics. African American women in the U.S. are about 40 percent more likely to die from breast cancer than white women, according to statistics from the Centers for Disease Control and Prevention. They are also more likely to be diagnosed at a younger age, and encounter more aggressive forms of the cancer.
“She has two girls, and I have two girls. Is it genetic?” Frazier asked. “Now we’re concerned about our girls. They’re still young. They’re in their 30s. I’m just praying that it doesn’t trickle down to them.”
Frazier’s concerns align with results from an initiative Susan G. Komen is conducting to reduce the breast cancer mortality rate for African American women. So far, the project has compiled data in the Portland metro area — including Vancouver — that shows African American women believe discrimination in the health care system is playing a role in the increased mortality rates.
Of 202 African American women ages 18-69 surveyed in the Portland metro area, 94 percent had health insurance. More than 80 percent knew about breast screening, how to self-check and said they think mammograms are necessary. However, only 66 percent said their interactions with health care workers made them want to return to the clinic, and more than a third said they didn’t hear about the importance of mammograms from their doctors.
The women said they experienced microaggressions from health care workers as well as reluctance from doctors to order screenings and mammograms for women younger than 40, even though African American women are diagnosed with more aggressive forms of breast cancer at an earlier age.
Frazier said she’s had family members encounter that problem.
“The doctors say you can’t get a mammogram. C’mon, change that,” Frazier said.
Another common problem among black women is not getting mammograms out of fear of detection, said D. Bora Harris, who worked on the data collection team for the project. Harris said that problem, combined with women who are reluctant to get screened because of discrimination they’ve encountered, leads to delays in checkups.
“A lot of African American women in our area are being treated and going in, but they’re not going as often as possible, as often as they should,” she said. “And many of them are really waiting until it’s too late.”
Kennedy said she thinks raising awareness about breast cancer is important, and in particular wants to make sure her family members get their breast screenings on schedule.
“Now that it’s over we just stopped talking about it,” Kennedy said. “It probably should be an ongoing conversation. There probably should be some follow-up, some discussions. Like we have the Sunday dinners. We need to do the same thing when it comes to breast cancer. Because it’s evident. It’s sitting right in front of us.”
A systemic problem
As helpful as raising awareness is, the disparities for African American women and breast cancer are part of a complex problem, tied to structural discrimination that African Americans face in the U.S., said Tomi Akinyemiju, an associate professor at Duke University in Durham, N.C.
“Disparities are something we need to address, not just as a moral issue, but also as a health care quality issue, as a cost issue. There’s more understanding now that this is a public health problem that we need to tackle,”Akinyemiju said. “When we look at disparities, we shouldn’t just say, ‘Oh, well, you know, they should just try to go to the hospital quicker.’ It’s a lot more complicated than that.”
As a social and molecular cancer epidemiologist with a focuses on health disparities, Akinyemiju has researched the mortality rate disparities as well as why black women more frequently encounter aggressive cancer subtypes relative to other racial groups.
Akinyemiju said that while cancer treatment has significantly improved over the past couple decades, disparities in outcomes still persist. Those disparities are, in part, connected to the quality of treatment African Americans receive in the U.S. medical system.
Since America has plundered African Americans through slavery, segregation, housing discrimination and disinvestment in communities, “most African Americans start off at a lower socioeconomic level than other groups,” Akinyemiju said.
“This lower status leads to poor access to care, meaning insurance that doesn’t really cover things, high out of pocket costs, lack of access to good care, including preventive care and screening, meaning that by the time the cancer gets diagnosed it’s usually at a later stage,” she continued. “Even after they are diagnosed, they still have suboptimal treatment because of all the access to care and financial issues.”
Yet, Akinyemiju explained those factors are really only the tip of the iceberg. She also explained that environment plays a role in health outcomes as well, and that it’s important to look beyond the “clinical aspects.”
There’s still ongoing research as to why African American women experience triple-negative breast cancer, an aggressive subtype, about twice as frequently as white women. Akinyemiju said that trend can’t necessarily be explained by socioeconomic status or access to care, but research she is currently conducting might point toward ancestry.
Akinyemiju said she has studied about 500 cases of Nigerian women with breast cancer, and while it’s a small sample size, they so far have rates of triple-negative breast cancer that are about twice as common as African American women in the U.S.
There is also research in neurobiology that shows general stress can have effects on biology and impact health outcomes, including with breast cancer, Akinyemiju said. A recent Harvard-led study showed current African American women with breast cancer, who were born in Southern states that once had Jim Crow laws — which legalized racial discrimination — were more at risk to contract tumors that have a worse prognosis.
Akinyemiju said stress related to living in toxic environments can lead to biological changes that might influence the development of more aggressive cancer subtypes. In other words, the discrimination that African American women face — for being African American and being women — might also affect the types of cancer they get.
“As a black person in the U.S., you are exposed to this daily, chronic stressor, having an impact on your biology, there’s not really a lot you can do to address that,” Akinyemiju said. “But if we understand the biological pathway through which those exposures may be affecting health outcomes, then maybe we can do something to target those pathways and improve outcomes.”
A merry ending
Darren Kennedy remembers having to answer questions about his wife’s breast cancer when friends and family would visit for the Sunday dinners. He didn’t like answering the questions. He said he knew his wife was struggling, but believed she would be OK. He had been through treatment with his mother, Rosa, but the diagnosis was still scary.
“I was in pain, and afraid of losing my best friend. The whole death part of it,” Darren Kennedy said.
Now that he and his wife are through treatment, they are going to renew their vows together in November at Colwood Golf Center in Portland. They met about 35 years ago at Jefferson High School in Portland. They’ve been married for 25 years. Now they want to celebrate the only way they know how: with family.
After their Sunday dinner in late September, Zsaneen Kennedy and her family sat in a circle in the living room. They discussed decorations for the ceremony, and who will sing. Darren Kennedy said that his father-in-law, John Frazier, scowled at him last time he walked down the aisle.
“Now we gotta go through that again,” John Frazier quipped.
Jokes aside, Darren Kennedy said he’s looking forward to the ceremony.
“We’ve seen a long journey,” he said. “As you go through things and grow, love looks a little different than it did 25 years ago. It’s just to remember my best friend.”