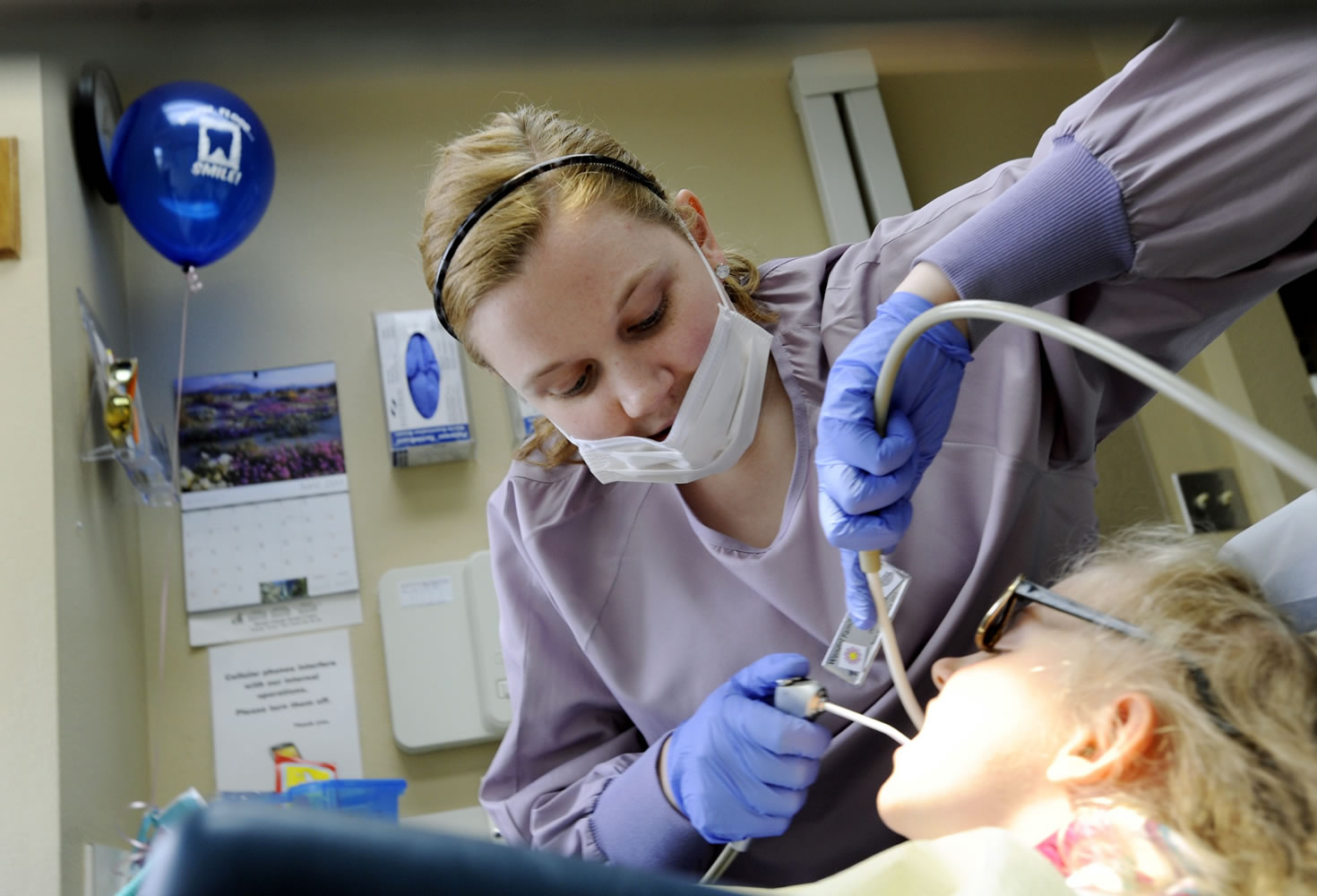
Hundreds of thousands of low-income Washington residents will soon have dental coverage.
Since January 2011, the state Health Care Authority has provided only emergency dental coverage for most adult Medicaid clients. Coverage included extractions, treatment of trauma-caused damage and temporary relief of pain or infection.
But beginning Jan. 1, the state will restore the adult dental benefits cut three years ago and provide the full slate of preventive and restorative dental care — services such as routine checkups, cleanings, fillings, root canals and dentures — for everyone on Medicaid.
“We’re just so happy the program was restored,” said Gail Baum, manager of the Medicaid dental program.
“You don’t know how hard it is to tell someone you can’t pay for this,” she said. “We’re supposed to be taking care of the whole person, and dental is a big part of that.”
Seniors who had both Medicare, which doesn’t offer dental coverage, and Medicaid and adults with disabilities were hit the hardest by the cutbacks, said Gail Kreiger, with the Health Care Authority. The reductions didn’t eliminate preventive dental care for children or most pregnant women.
“The worst calls I received were those clients that had teeth that were causing pain, that were most likely infected, but they didn’t want to have them pulled because there was nothing in return,” Baum said.
Many of the program’s clients are living on limited incomes, $600 to $700 a month. The most inexpensive dentures still cost nearly $1,000, Baum said.
Once restorative services are restored Jan. 1, the state expects to see a wave of people requesting dentures.
When the services were eliminated, about 105,000 adults were utilizing the program, said Jim Stevenson, spokesman for the Health Care Authority. But the state has about 400,000 adult Medicaid clients, all of whom could potentially use the services, he said.
“Most of our adult clients realized they had a dental benefit when it was cut,” Stevenson said. “So it just got a lot more visibility.”
The state budgeted about $23.3 million for the biennium to pay for adult dental services. The federal government will provide another $49.2 million, largely because of the state’s Medicaid expansion rolling out Jan. 1. The Medicaid expansion will add an estimated 270,000 adults by the end of the biennium, Stevenson said.
As a result of the cutbacks, the Free Clinic of Southwest Washington has seen a dramatic increase in people seeking care. Since January 2011, the Free Clinic’s adult dental visits have increased 74 percent, said Barbe West, executive director of the Free Clinic.
The clinic offers three to four half-day adult dental clinics each week, each staffed by volunteer dentists and hygienists. But for every person who is treated, another name is added to the list. The Free Clinic’s waiting list currently has 440 names. Most are seen within three months.
“We have really tried,” West said. “We haven’t been able to absorb it.”
The clinic has implemented a few changes to help work through the list more quickly. For example, a dental hygienist now screens everyone on the waiting list before they receive an appointment. That way, West said, the clinic can be sure the patient is seeing a dentist with the skill set to treat him or her.
The screening also allows the clinic to prioritize patients who have severe dental problems. Those patients are typically seen within two to three weeks, West said.
In addition, the clinic has worked with local dentists to provide services. About 30 dentists have agreements with the clinic to treat between two and 10 Free Clinic patients each year, West said.
And while West said she’s thrilled the state is restoring dental services, she’s also hesitant to celebrate. She’s worried dentists won’t accept Medicaid clients.
That’s a legitimate concern, according to Dr. Kristine Aadland, who runs her own practice and is president of the Clark County Dental Society. Many dentists were frustrated by the low reimbursement rates for Medicaid clients and the often lengthy wait for payment, she said.
“The reimbursement rate doesn’t even really cover our costs,” Aadland said.
For example, Aadland charges $250 for a standard filling. Medicaid reimbursed the dentist $62, she said. That didn’t even cover half of the $150 cost to provide the treatment, Aadland said.
For cleanings, dental offices were reimbursed $36. The hourly wage of a dental hygienist performing the work is between $34 and $36, Aadland said.
Aadland won’t be accepting Medicaid clients once services are restored. Her practice is too busy and she can’t afford the added billing work and treating people for less than the cost of the service, she said.
Many other local dentists are waiting to see whether reimbursement rates are improved and what services the program will cover before deciding to accept Medicaid patients, Aadland said.
Stevenson, with the Health Care Authority, said the reimbursement rates will be the same in January as they were before the services were canceled in 2010.