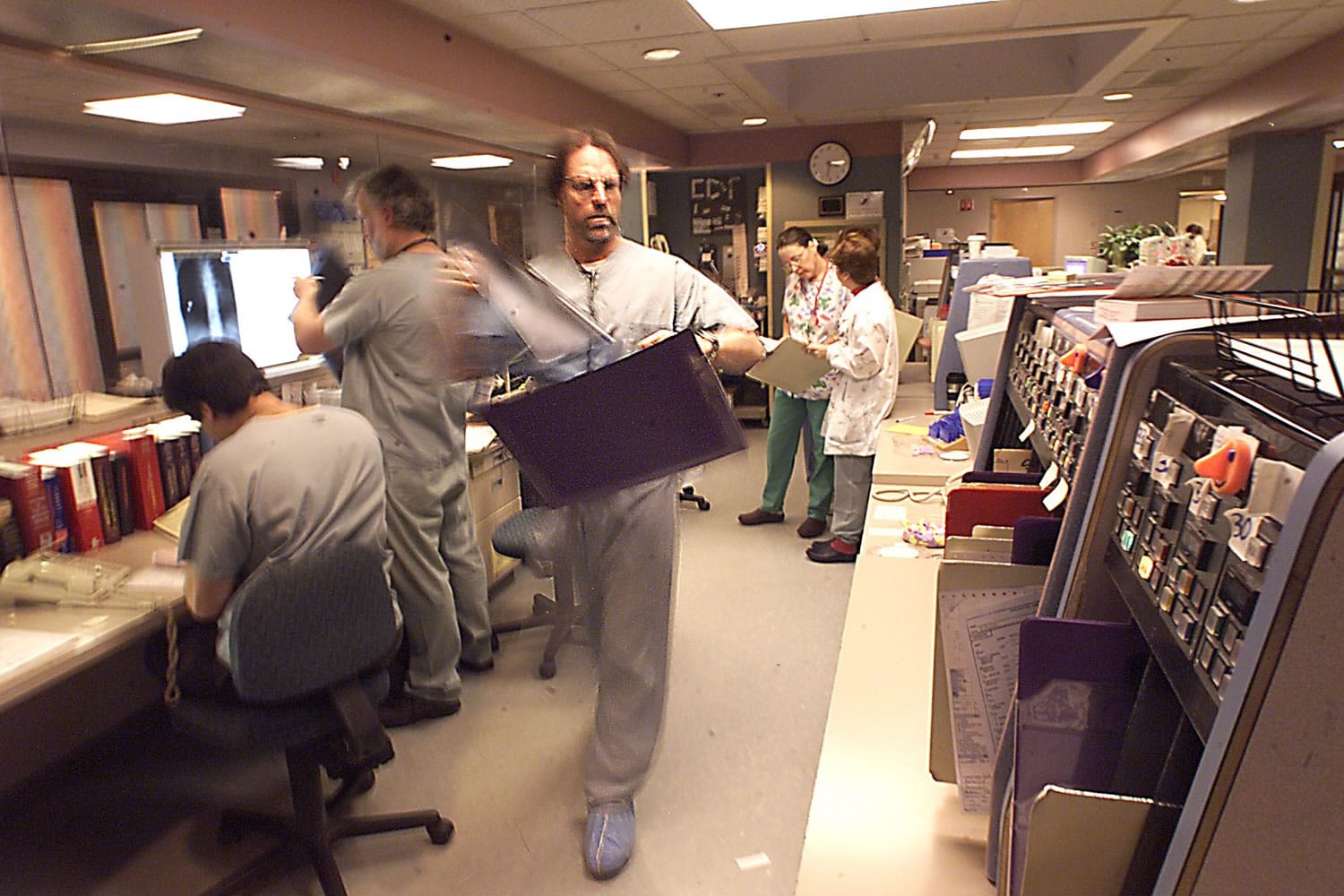
The state’s plan to limit the number of times Medicaid patients can visit hospital emergency departments for non-emergencies has been halted.
At least for now.
Last week, Thurston County Superior Court Judge Paula Casey stopped the state’s implementation of a rule limiting Medicaid patients to three non-emergent visits per year to hospital emergency departments.
o Last year, the Washington State Health Care Authority spent nearly $98 million on 327,965 fee-for-service Medicaid emergency department visits. That’s an average of $299 per visit.
The Washington State Health Care Authority — which oversees Medicaid and six other health care programs — implemented the rule as part of a legislative mandate to cut the Medicaid budget. The rule, which went into effect Oct. 1, was expected to save more than $30 million from its implementation date to the end of the biennium on June 30, 2013.
The state told patients if they exceeded the limit, they could be billed for the services.
The Health Care Authority drafted a list of 700 diagnoses classified as non-emergent. The list included some conditions that could be true emergencies or perceived as emergencies, such as chest pain, abdominal pain and miscarriage.
That list drew criticism from physicians and hospitals across the state and prompted several organizations to file a joint lawsuit against the state.
Last week, Casey sided with the professional groups and found the state failed to follow proper rule-making procedures.
While the ruling will halt the implementation, physicians don’t expect it will prevent the change from going into effect later.
“It’s just kind of a pause in the process and see if the decision that was made was a valid one or if we need to modify it,” said Dr. Marty Bell, director of emergency medicine at PeaceHealth Southwest Medical Center.
The state will now have to go through a formal rule-making process that will likely include public hearings. Health Care Authority spokesman Jim Stevenson said state officials will consider comments from the public, providers and hospitals as they move forward.
“We’re under a legislative directive to put that rule in effect,” Stevenson said. “It’s clear that would be our intent, but we want to follow the process carefully and take in account the experience we’ve had.”
Bell said he hopes the Health Care Authority will re-evaluate the diagnoses list as part of the process. The diagnoses are too broad and many could be construed as true medical emergencies, he said.
“Some of those patients could avoid making reasonable decisions and put themselves at risk of more serious illness or even death,” Bell said.
Dr. Michael Albrich, medical director for emergency services at Legacy Salmon Creek Medical Center, agreed the diagnoses list was cause for concern. He’s also concerned future Medicaid cuts could further impact hospital emergency departments.
“If Medicaid undercuts services in the community, that could lead to increased emergency department visits,” Albrich said. “That will be very counterproductive. It will essentially defeat the work they’re trying to do with the three-visit limit.”
The limit was implemented as an effort to direct patients to primary care providers, rather than more expensive emergency departments, for non-emergent services, according to the Health Care Authority. Only 3 percent of the state’s Medicaid population makes more than three visits a year to emergency departments. That small group of clients runs up large numbers of visits each year, some exceeding 100, usually in search of pain medication, according to the state.
Bell said he would rather see the state’s efforts geared at educating patients about how to access primary care providers rather than limiting emergency department visits.
“I think the fact that there was a unilateral decision made merely to bridge the budget gap, it really didn’t take into account the frontline reality of the day-to-day decisions we have to make and patients have to make,” Bell said.
Marissa Harshman: http://twitter.com/col_health; http://facebook.com/reporterharshman; marissa.harshman@columbian.com; 360-735-4546.