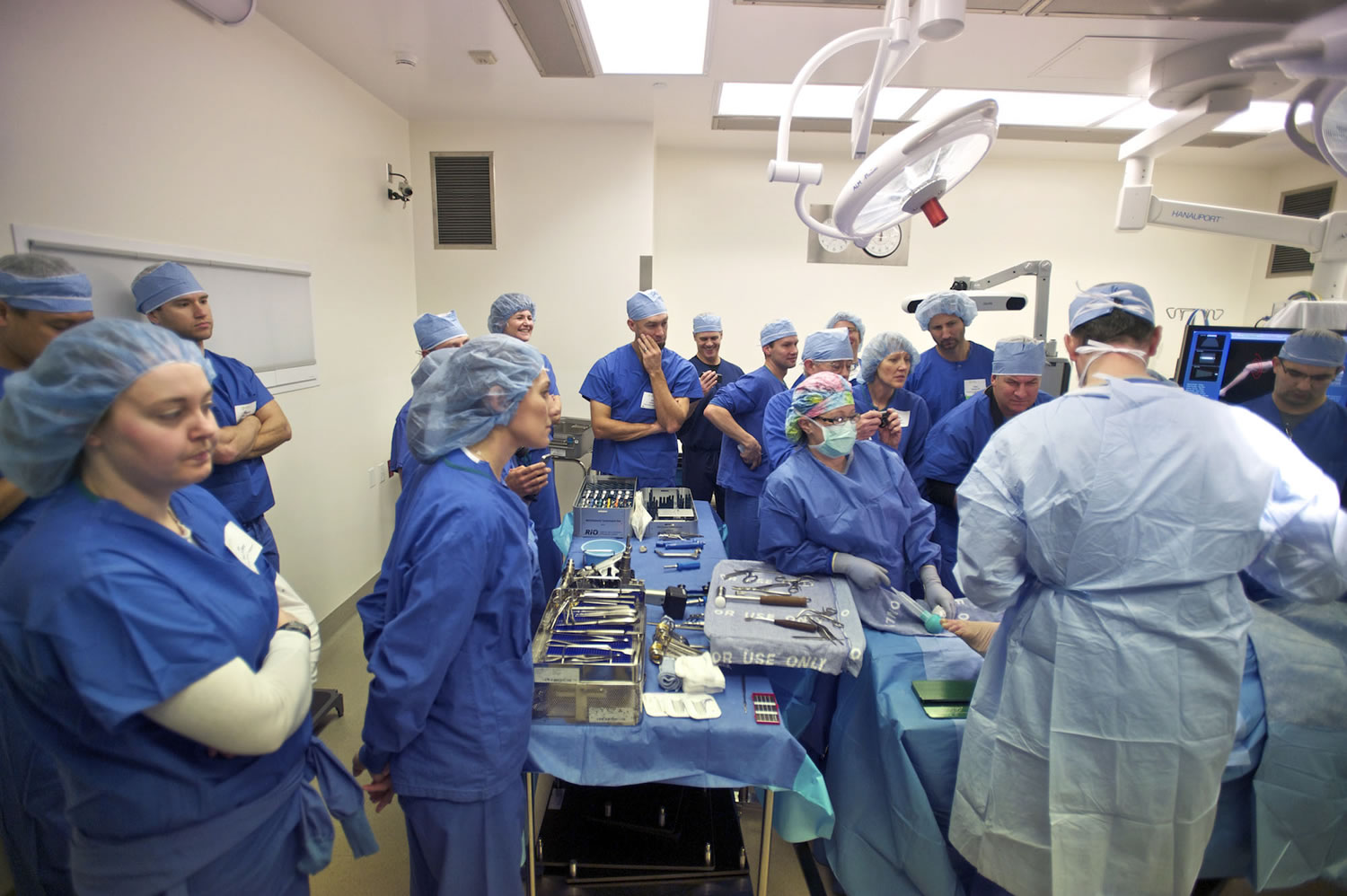
As a group of physical therapists took turns at the operating table, their faces showed a combination of wonder, fascination, and a bit of squeamishness.
Each tried his or her hand during a demonstration knee surgery, performed on a cadaver leg. But it wasn’t just human hands at work for this partial knee replacement. They worked with the guidance of a robotic arm that already knew where to go.
Dr. Todd Borus, the surgeon leading the demonstration at Legacy Salmon Creek Medical Center on Saturday, explained it this way:
“It won’t let me color outside the lines,” he said.
Legacy Salmon Creek was the first hospital in the region to offer the robotic-assisted procedure, known as MAKOplasty, in 2009. It’s still one of just three facilities in the Portland-Vancouver area using the technology. Borus himself has performed more than 500 such procedures.
MAKOplasty relies on computer modeling to create a 3-D image of the patient’s knee before the operation begins. Once in surgery, sensors mark various points on the bone structure to make sure everything matches up properly.
On Saturday, Borus flexed the cadaver leg during the procedure. The visiting therapists watched a monitor as an animation of the knee moved with it in real time.
The robotic arm uses a drill-like tool to remove bone and cartilage, but only in a defined area mapped by the computer model. Try to move the arm outside that area, and it will stop itself.
“No matter how good you are as a surgeon, the robotic arm can help you,” Borus said.
The procedure is used for partial knee replacement, and offers a less-invasive alternative to a total knee replacement, according to Legacy. Resurfacing is limited only to the diseased portion of the knee, after which an implant is inserted for better movement. The process allows for a smaller incision, less trauma and a faster recovery time, Borus said.
Observing Saturday was a group from the Oregon Physical Therapy Association. As physical therapists, they’re the ones who often see patients after they leave the operating room.
“Not all surgical procedures are created equal,” said Thomas Fliss, a physical therapist who practices in The Dalles, Ore. “It’s exciting to see what goes on behind the scenes on the good outcomes.”
A grant has allowed Legacy to track the long-term outcomes of MAKOplasty procedures, Borus said. Two years after the operation, about 90 percent of patients counted themselves as satisfied or very satisfied, he said.
Patients with osteoarthritis can be candidates for MAKOplasty partial knee replacement. Many patients who undergo the procedure are in their 50s or 60s, but the total age range is much wider than that, Borus said. The technology can also be used for hip replacements.
Saturday’s group also observed a demonstration of a shoulder procedure at Legacy. The Oregon Physical Therapy Association has organized a series of similar visits elsewhere to stay connected with the latest in the medical and surgical field, said board member Tom Moline.
“These are our patients,” Moline said. “We want to know what’s going on.”